According to the National Kidney Foundation, tests are recommended for the treatment of chronic kidney disease.
- Measuring blood pressure. Blood pressure levels are not only a factor in causing kidney disease, but indicate the presence of kidney disease.
- Measuring serum creatinine levels to provide for a calculation of glomerular filtration rate (GFR).
- Testing urine is very important for the presence of albumin or other proteins.
If these tests show an indication of kidney disease, your health care provider may order additional testing. These include imaging tests like magnetic resonance imaging (MRI), ultrasound tests, and CT scans etc.
How The Tests Are Done?
1. Blood Tests
- This test measures the levels of a waste product called creatinine in the blood.
- The doctor uses your blood test results to calculate how many ml of waste your kidneys should be able to filter per minute.
- This calculation called as your estimated glomerular filtration rate (eGFR).
- A pair of Healthy kidneys must filter more than 90ml/min.
- eGFR (estimated glomerular filtration rate)
The eGFR indicates how well your kidneys are cleaning your blood.
The main function is that your body makes waste all the time and this waste goes into your blood. Healthy kidneys usually take the waste out of your blood. One type of waste is creatinine. When you have too much level of creatinine in your blood, it might be a sign that your kidneys are having trouble filtering your blood.
The blood test is done to find out how much creatinine is in your blood. If your eGFR is less than 60 for 3 months or more, you might have kidney disease.
2. Urine Tests

This test is performed to check if there is blood or protein in your urine. If your urine contains blood or protein, it may be a sign that your kidneys are not working well.
3. Blood Pressure Tests
High blood pressure can cause kidney disease, but at the same time kidney disease can also cause high blood pressure. For most people, normal blood pressure should be or less than 120/80.
Who Should Be Tested For CKD?

You must visit a nephrologist or a general doctor at least if you have persistent symptoms of CKD, such as:
- weight loss
- poor appetite
- swollen ankles, feet, or hands
- shortness of breath
- tiredness
- blood in urine
- peeing more than usual, particularly at night
- Your GP can check for other possible causes and arrange tests accordingly
Because CKD often has no symptoms in the initial stages, some people at a higher risk should be checked on a regular basis.
Precautionary Measures

Regular testing is important and should be done if you have:
- Heart diseases
- kidney stones, enlarged prostate, or lupus
- a family history of advanced CKD. You’re also more likely to develop kidney disease if you’re black or of south Asian origin.
- high blood pressure
- diabetes
- acute kidney injury
- protein or blood in your urine
- People taking long-term medicines that can affect the kidneys, such as lithium, or non-steroidal anti-inflammatory drugs (NSAIDs), should also be tested regularly.
Treatment For Chronic Kidney Disease
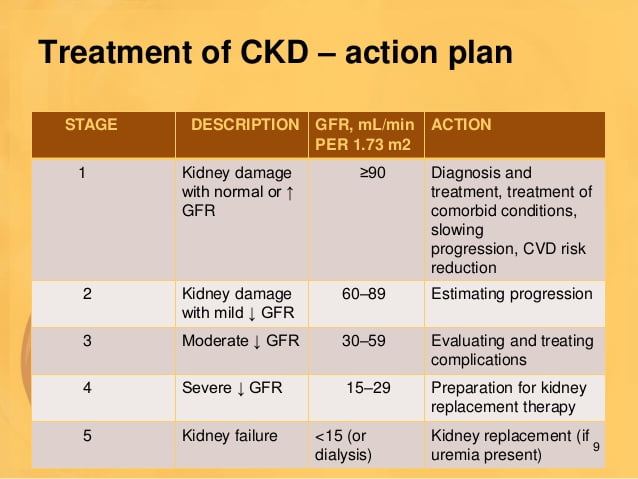
It focuses on slowing the progression of the kidney damage, usually by controlling the underlying cause. Chronic kidney disease can gradually progress towards end-stage kidney failure, which is fatal without dialysis or a kidney transplant. Damage to your kidneys is usually permanent. But you can take important steps to keep your kidneys healthy r as long as possible by
- Controlling your blood sugar level
- Keeping a healthy blood pressure
- Following a low-salt and low-fat diet
- Keeping a healthy weight
- Restrict your smoking
- Limiting alcohol
- Light to moderate exercising at least 30 minutes 5 days a week
- Talking to your doctor
Treating Complications


- High blood pressure medications. People with kidney disease experience high blood pressure. Your doctor may recommend medications to lower your blood pressure like angiotensin-converting enzyme (ACE) inhibitors or angiotensin II receptor blockers and to preserve kidney function.
- Medications to treat anemia. The doctor might recommend supplements of the hormone erythropoietin with added iron as these help in the production of more red blood cells, which relieve fatigue and weakness associated with anemia.
- Medications to relieve swelling. DIURETICS helps to maintain fluid balance in your body.
- Medications to lower cholesterol levels. People with chronic kidney disease experience high levels of LDL or bad cholesterol, which can increase the risk of heart disease.
- Medications to protect your bones. Your doctor will prescribe calcium and vitamin D supplements to prevent weak bones and lower your risk of fractures.
- Low protein diet
- The body processes protein from foods, it creates waste products that your kidneys must filter from your blood. You must visit a dietitian who can suggest remedies and ways to lower your protein intake.
Treatment for end-stage kidney disease
When your kidneys are unable to keep up with the wastes and fluid clearance on their own and you develop complete kidney failure, you have end-stage kidney disease. Then you need
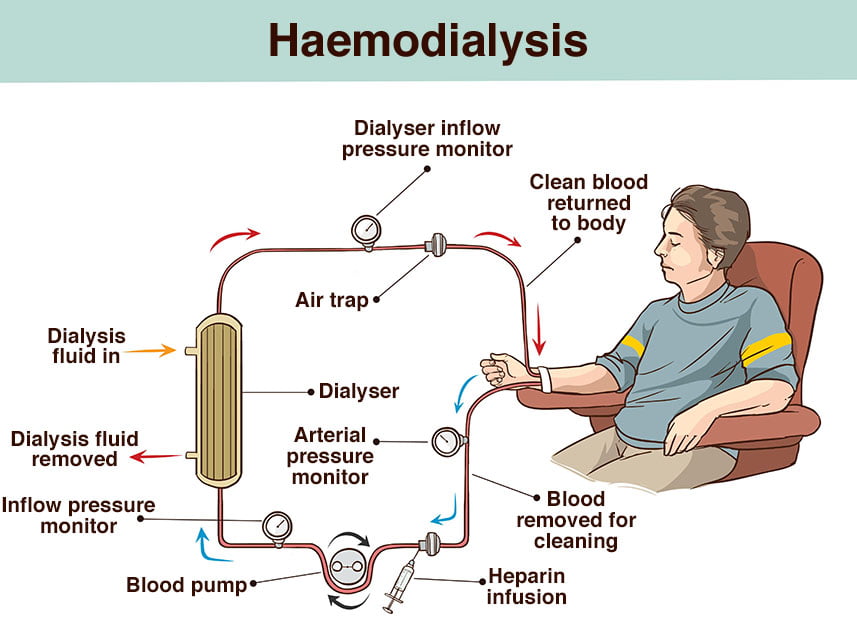
- Dialysis artificially removes waste products and extra fluid from your blood when your kidneys can no longer functional to do this.
- In haemodialysis, a machine is used which filters waste and excess fluids from your blood.
- In peritoneal dialysis, a thin tube inserted into your abdomen and then fills your abdominal cavity with a dialysis solution that absorbs the wastes as well as fluids. Then the dialysis solution drains from your body, carrying the waste along with it.
- Kidney transplant – It involves surgically placing a healthy kidney from a donor man into your body.
Potential future treatments
Regenerative medications have the potential to fully heal damaged tissues and organs, and provide hope for people who have worse conditions.
Regenerative medicine approaches include:
- Powering up the body’s natural ability to heal itself
- Using the body’s healthy cells, tissues or organs from a living or a deceased donor to replace the damaged ones







